The air in the waiting room didn't smell like antiseptic. It smelled like warm bodies, damp coats, and the low-frequency hum of collective anxiety. In a small clinic outside of Columbia, South Carolina, a mother held her toddler, watching the way his chest rose and fell in jagged, shallow increments. She wasn't thinking about epidemiological curves or the resurgence of preventable diseases. She was thinking about the heat radiating off his skin—a dry, baking heat that felt like it could singe the sheets.
Then came the spots.
They started behind the ears, a faint dusting of pink that looked almost like a heat rash. Within hours, they had marched across his face and neck, merging into a map of inflammation that consumed his small frame. This was not a ghost story from the nineteenth century. This was the reality for nearly 1,000 families across South Carolina over the last several months.
Measles is a quiet thief. It lingers in the air of a room for two hours after an infected person has left, waiting for the next pair of lungs. It is perhaps the most contagious viral hunter known to man. If one person has it, nine out of ten people close to them will catch it if they aren't protected.
The state has finally declared the outbreak over. The tallies are settled. The hospital wings have emptied. But to look at the numbers—984 confirmed cases—is to miss the marrow of the story.
The Geometry of a Contagion
Think of a single spark dropped into a field of dry tallgrass. If the grass is green and lush with moisture, the spark dies. In the world of public health, that moisture is "herd immunity." When 95% of a population is vaccinated, the virus finds nowhere to land. It hits a wall of protected immune systems and fizzles out.
In certain pockets of South Carolina, the grass had turned to tinder.
Vaccination rates in specific school districts had dipped just enough to create a draft. When the first case arrived—likely a traveler returning from a region where the virus still circulates freely—the spark found its fuel. What followed was a geometric explosion. One case became five. Five became twenty-five. By the time the Department of Health and Environmental Control (DHEC) could mobilize, the virus was already three steps ahead, hiding in grocery store aisles, church pews, and daycare centers.
For the average adult, a fever is an inconvenience. For a child with measles, it is a physiological assault. The virus doesn't just cause a rash; it causes a temporary "immune amnesia." It wipes the hard drive of the body’s immune memory, deleting the instructions on how to fight off other illnesses. For months, or even years after the spots fade, these thousand children remain vulnerable to every other bug that passes through their classroom.
The Cost of a Breath
We often talk about the "cost" of healthcare in the abstract—insurance premiums, tax brackets, state budgets. We rarely talk about the cost of a parent missing three weeks of work because their child is quarantined. We don't see the hourly-wage worker choosing between a paycheck and staying home to ensure their daughter’s fever doesn't spike into a seizure.
During the height of the South Carolina outbreak, the pressure on local pediatricians was immense. Waiting rooms became tactical zones. If a parent called in reporting a high fever and a cough, they were told to stay in their cars. Doctors would suit up in N95 masks and face shields, meeting patients in the parking lot to swab throats through half-rolled windows.
It felt like a regression.
Modern medicine has spoiled us. We have forgotten what it looks like when a child loses their hearing because of a measles-related ear infection. We have forgotten the terrifying stillness of viral encephalitis. Because we haven't seen these things in decades, we began to treat the threat as a myth. We started to believe that the absence of the disease was a natural state of being, rather than a hard-won fortress maintained by needles and glass vials.
The Invisible Stakes
The most heart-wrenching part of this nearly thousand-person tallgate wasn't the children who were old enough to be vaccinated but weren't. It was the ones who had no choice.
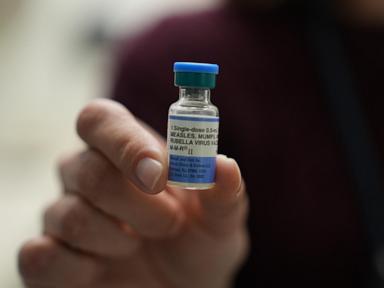
Consider the "infant window." Babies cannot receive the MMR vaccine until they are twelve months old. For the first year of their lives, they are entirely dependent on the people around them to act as a human shield. In this outbreak, dozens of infants under the age of one ended up in respiratory distress, their tiny bodies struggling to process a virus they were never meant to encounter.
Then there are the "shadow patients." These are the people undergoing chemotherapy, the organ transplant recipients, and the elderly whose immune systems have grown brittle. They did everything right. They followed every protocol. Yet, they found themselves trapped in their homes, terrified to go to the pharmacy or the library because the air itself had become a gamble.
The outbreak didn't just sicken people; it eroded the social contract. It turned neighbors into potential vectors. It made the simple act of breathing in a public space a moment of silent calculation.
The Reckoning
The state's response was a massive, grinding machine of contact tracing. Health officials spent thousands of hours on the phone, reconstructing the movements of the infected. Where did you shop on Tuesday? Who sat next to your son at the basketball game? Did you go to the post office? Each answer spawned ten more calls. Each call resulted in more people being told to stay home, to wait, to watch for the telltale cough. It was a monumental effort that eventually choked the virus of its oxygen. By isolating the susceptible and surging vaccine clinics into the most affected zip codes, the "firefighters" of the public health world finally managed to beat back the flames.
But the "end" of an outbreak is a deceptive term.
While the official count has stopped, the trauma lingers. There are parents in Greenville and Charleston who still jump every time their child feels a little warm to the touch. There are teachers who spent months scrubbing desks with a frantic intensity, wondering if they would be the ones to carry the virus home to their own families.
The silence that has returned to the clinics isn't the silence of peace. It’s the silence of a temporary truce.
The Lesson in the Linens
The virus is not gone from the earth. It is merely waiting. It exists in a state of permanent hunger, circling the edges of our communities, looking for the next gap in the fence.
We live in a world that prizes individual autonomy above almost all else. We want to make our own choices, live our own truths, and govern our own bodies. But a virus doesn't care about philosophy. It is a biological machine designed to find a host. It exploits our interconnectedness. It uses our love for one another—the way we hug, the way we huddle together in grief or celebration—as a highway.
The South Carolina outbreak was a warning shot across the bow of a society that has grown complacent. It reminded us that our health is not a solo venture. We are all breathing the same air, walking the same aisles, and touching the same doorknobs.
When the last child in this outbreak finally saw their fever break, and the red spots began to turn to brown, flaky patches before disappearing, a family somewhere felt a profound sense of relief. They likely stripped the sweat-soaked sheets from the bed and threw them in the wash, wanting to erase every physical trace of the ordeal. They wanted to go back to normal.
But normal is a fragile thing. It is a thin crust over a very deep well.
The next spark is already in the air, drifting toward the next field of tallgrass. Whether it catches or dies depends entirely on how much we value the invisible shield we build for one another. The outbreak is over, but the air is still there, shared by us all, waiting for the next breath.
The spots have faded, but the vulnerability remains etched into the map.